Colon cancer deaths concentrate in one group
New data show rising colon cancer mortality concentrated among younger adults, particularly men, while older groups benefit from screening and better treatment.

New data show rising colon cancer mortality concentrated among younger adults, particularly men, while older groups benefit from screening and better treatment.

Pragmata’s eerie, low-orbit isolation has clear cousins in five surreal sci-fi anime that mix cosmic dread, fragile humanity and brutal visual imagination.
2026-04-19
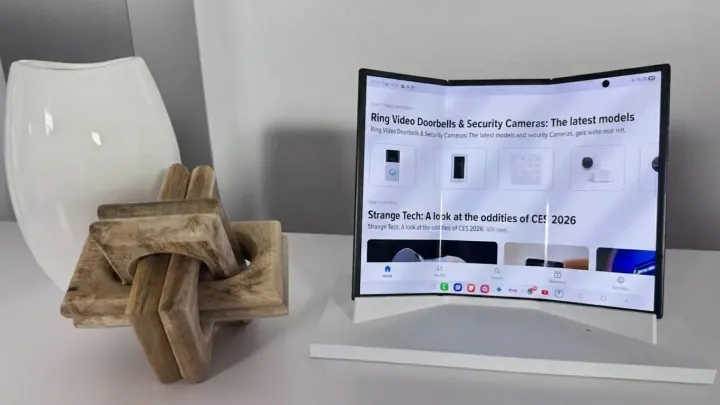
Samsung’s experimental Galaxy Z TriFold has sold out its restricted run, signaling a controlled, one‑off showcase rather than a mass‑market product line.
2026-04-19

With e‑bike injuries and deaths climbing, cities are moving toward registration, tighter regulation and redesigned infrastructure to manage speed, mixing of vehicles and lithium‑ion risk.
2026-04-19
A major U.S. cohort study reports that never-married adults have substantially higher cancer risk, especially for preventable tumors, likely driven by smoking, alcohol, obesity, and social isolation.
2026-04-19

A long-awaited birth nearly ended in tragedy when Casey Gould noticed a disturbing sign and voiced, “I think I’m about to die,” exposing how fast obstetric emergencies can escalate.
2026-04-19
A Welsh patient, dismissed for years by clinicians, used ChatGPT and obtained in minutes a rare disease hypothesis that later aligned with specialist findings, raising questions about AI in front‑line diagnosis.
2026-04-19

Arc Raiders is reshaping Expeditions so skill points now scale with damage dealt, while a new Expedition Window adds tuned rewards, tweaks to enemy pressure, and a clearer grind for progression.
2026-04-19

Tomodachi Life: Living the Dream sidesteps Animal Crossing: New Horizons’ burnout loop by replacing obligation-driven chores with self-running social drama.
2026-04-19

Samsung will ship One UI 8.5 to many current Galaxy phones, backporting several Galaxy S26 software features as a free upgrade.
2026-04-19

Amazon’s latest Fire TV Sticks block sideloading, hardening the platform around its own Appstore and raising fresh questions over user choice, control, and antitrust risk.
2026-04-18