A Welsh patient, dismissed for years by clinicians, used ChatGPT and obtained in minutes a rare disease hypothesis that later aligned with specialist findings, raising questions about AI in front‑line diagnosis.
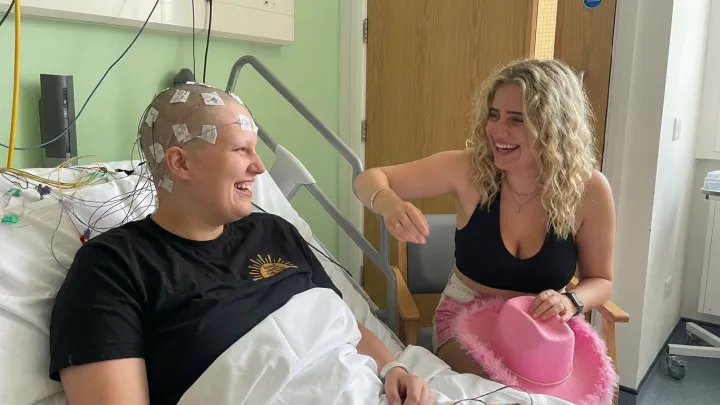
Silence in the clinic can be louder than any alarm, and that silence defined the long search for answers to Phoebe Tesoriere’s worsening pain and fatigue. Tests came back “normal,” referral letters circled between departments, and each appointment reset the clock while her symptoms advanced, an all too familiar pattern for patients with rare disease profiles.
The unsettling part is simple. A general‑purpose chatbot did what multiple consultations did not. Out of frustration, the twenty‑three‑year‑old from Wales fed ChatGPT a detailed history: stabbing joint pain, episodes of dizziness, gastrointestinal distress, and a family record hinting at autoimmune pathology. The system, trained on massive corpora of clinical literature and case reports, returned a short list of possibilities that included a connective tissue disorder and a form of postural orthostatic tachycardia syndrome, both often missed without targeted autonomic testing.
This reversal of roles should worry clinicians even as it intrigues them. Armed with the AI‑generated differentials, Tesoriere pressed for specific investigations, including tilt‑table assessment and immunological panels, which moved her case out of the vague category of “medically unexplained” and toward defined diagnostic codes. Specialists later confirmed conditions that closely matched the chatbot’s early suggestions, turning an online query into a practical roadmap for care and a pointed critique of how human systems handle complex cases.
What her story exposes is less machine brilliance than a structural gap: overloaded primary care, limited appointment slots, and cognitive bias toward common conditions. In that gap, a free tool sifted published evidence without fatigue or hierarchy, leaving medicine to decide whether such systems should stay a last‑ditch workaround for desperate patients or become a formally integrated, audited layer in the workup of rare and chronic illness.