
Three Medical Routines Older Adults Can Skip
Researchers argue that certain cancer screenings, tight diabetes control and routine bone density scans bring more harm than benefit for many older adults.

Researchers argue that certain cancer screenings, tight diabetes control and routine bone density scans bring more harm than benefit for many older adults.

Ask.com is shutting down its core search engine as owner IAC ends investment in search and shifts the site toward Q&A and media tie-ins.
2026-05-03

Crimson Desert patch 1.5 adds a full boss rematch system, re-blockades, legendary creature pets, and NVIDIA DLSS MFG support as Pearl Abyss builds on 5M sales.
2026-05-03

Motorola’s Razr Ultra debuts a carbon-silicon battery in a U.S.-focused flagship, promising higher energy density and faster charging as it challenges Apple and Samsung.
2026-05-03

Longevity hype oversells clock‑rewinding; experts argue the real health gain comes from technology that prevents and treats chronic disease.
2026-05-03
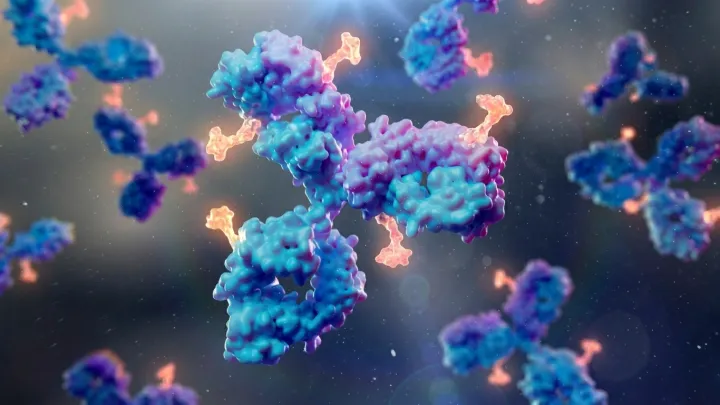
Researchers report an engineered antibody that neutralizes a virus infecting roughly 95% of people, blocking entry into host cells and reshaping vaccine and therapy prospects.
2026-05-03
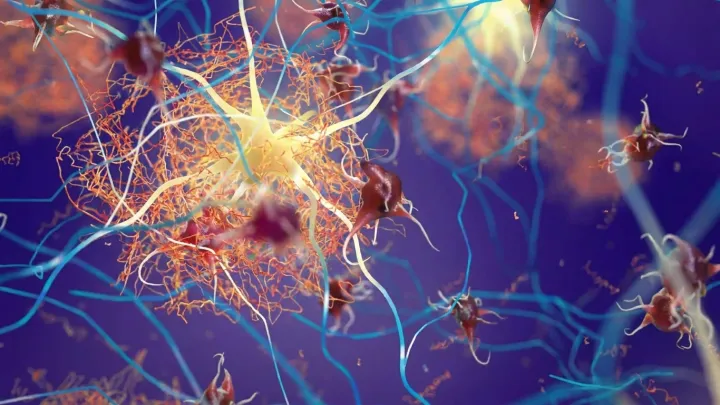
Raising the protein Sox9 in astrocytes helps the brain clear Alzheimer’s plaques and preserves memory in mice already showing cognitive decline.
2026-05-03

Hair shedding tied to GLP-1 weight-loss drugs is turning a side effect into a fast-growing, premium market for pharmaceutical and cosmetic hair treatments.
2026-05-03

Nintendo’s Shigeru Miyamoto argues the rapid pace of The Super Mario Galaxy Movie mirrors game design, trading character pauses for dense visual action to hold broad, impatient audiences.
2026-05-03

Hospitals across New York and New Jersey are running biothreat drills, surge plans and multilingual triage to prepare for infectious diseases linked to incoming World Cup fans.
2026-05-03

SteamOS gains have exposed Windows gaming weakness, yet soaring RAM demands in modern titles now stall defections and hand Microsoft a breathing window.
2026-05-02